Diaphragmatic breathing is essentially deep breathing. Regularly performing diaphragmatic breathing builds awareness of the deep core and calms the body, biasing it towards the parasympathetic nervous system, aka the “rest and digest” branch. It can be one of our first defenses to managing pain.
It’s the link between our conscious minds and our body’s automatic functions. Automatic functions are controlled by the autonomic nervous system. They are functions you don’t have to think about to perform, such as heart rate, temperature, and digestion. When your body becomes dysregulated, say when you have an anxiety attack, your body responds as if it is under a physical threat. Your “fight or flight” response kicks in and your physiology drastically changes. These changes are meant to keep you safe, however, in a chronic state they can do more damage than good. We can mitigate damages by communicating with our body through slow and controlled breathing.
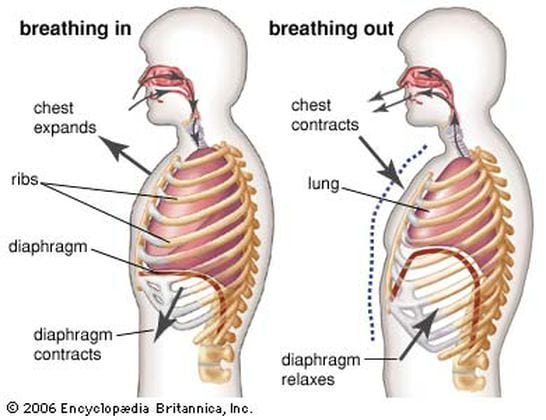
How To Perform Diaphragmatic breathing
You can perform deep breathing exercises in any position at any time of day. If you have trouble connecting with your breath, however, initially try practicing while laying down in a quiet place to increase focus and awareness until you get the hang of it.
Setup
- Find a comfortable place to lie down on your back.
- Place one hand on your chest and one below your rib cage on your abdomen.
- Breath in deeply through your nose. Feel your belly rise.
- Exhale fully through your mouth. Feel your belly lower.
- Perform for 2-5 minutes.
- Notice how your body feels before and after.
Tips
Focus on expanding your belly. You should feel minimal movement in your upper chest. Slow your breathing by:
- Counting: Count slowly to 4 on the inhale, hold for a count of 4, then exhale for a count of 8.
- Mantra: You can use any mantra you choose. For example, inhale “I am” exhale “calm”.
- Imagery: Firstly, imagine the air entering your body and filling up all your body. Then, visualize it emptying out slowly through your mouth. Imagine a color to the inhaled versus exhaled air, such as red and blue.
- Guided Breathing: Check out your app store by searching breathing apps or google “guided breathing”. There are endless possibilities, so find what works for you. Some commonly used apps are Calm, Headspace, Liberate, and iBreathe.