Tongue Ties, TOTs, OMT, and a Partridge in a Pear Tree!
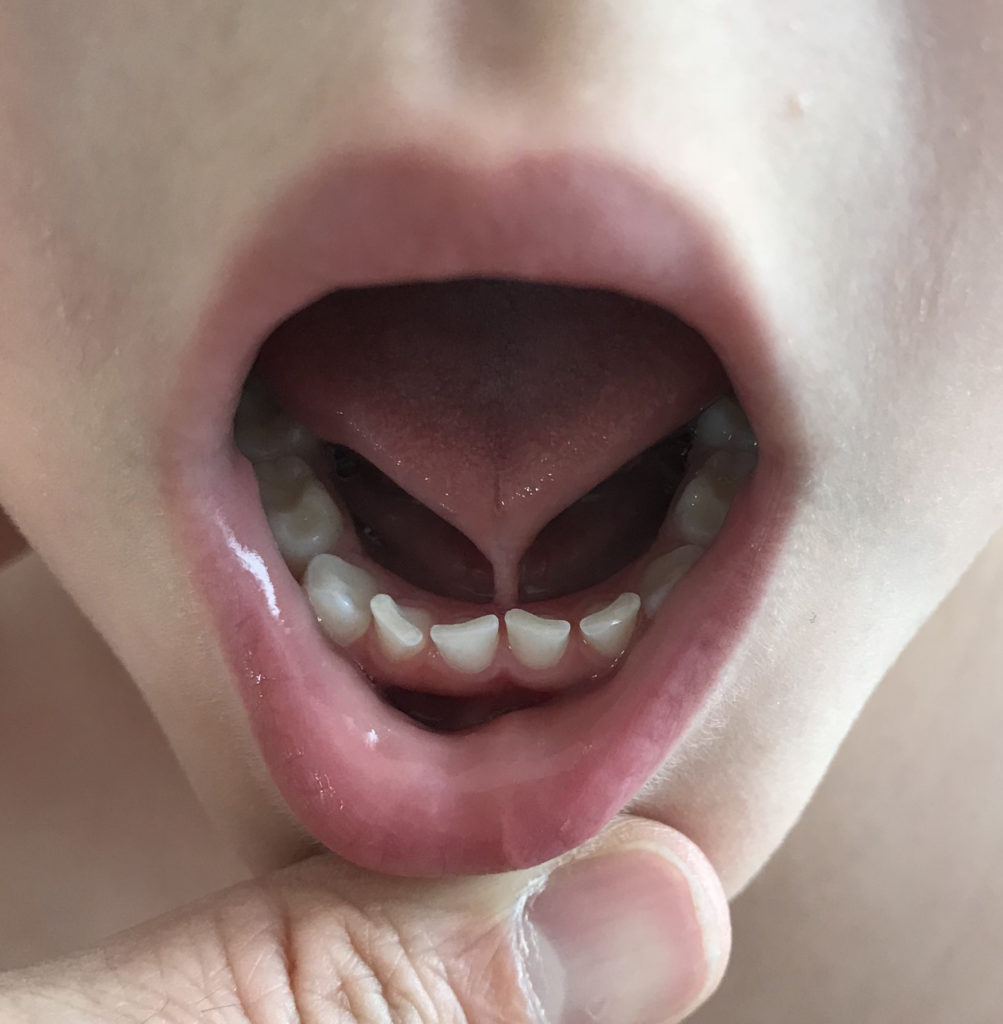
It seems everywhere you look, we are a nation obsessed with tongue ties. But why? What is the great debate? Let’s break it down.
“The reason we’re hearing about tongue-tie more now is that the last 10 to 11 years have demonstrated that the part of the tongue responsible for suction is the middle of the tongue, not the tip,” says Bobby Ghaheri, MD (otolaryngologist). This research refers to the part of the tongue restricted by a posterior tongue tie which Ghaheri states is “still under the front of the tongue but less visible.” Hence the name, posterior tongue tie. Frena is a small band of tissue that extends from the floor of the mouth to the bottom of the tongue. In addition to tongue ties, tethered oral tissue (TOTs) can define six other oral frena located bilaterally, in the upper and lower buccal cavities or cheeks, and upper and lower lips. Frena can either support movement or restrict it. However, frena cannot be stretched due to their collagen make up.
What is a Tongue Tie?
A tongue tie, or ankyloglossia, will present as an overly short or thick frenulum that restricts the tongue’s movement. Similarly, a lip tie can occur as well as buccal cavity ties. There are different classifications of each, however assessing function is what drives treatment or intervention.
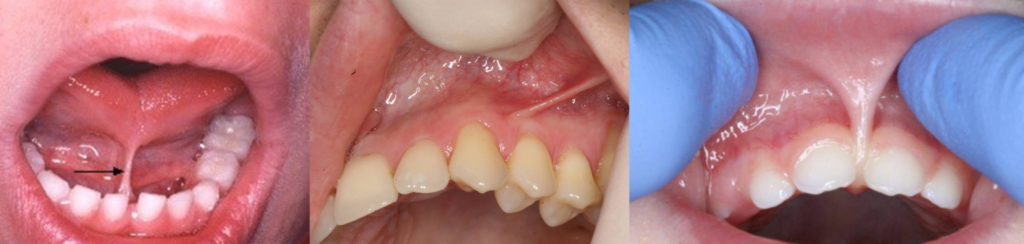
Signs of TOTs in infancy may include difficulty breastfeeding causing failure to thrive and/or maternal pain. It can also be an issue causing “picky” eating or difficulty transitioning to solids. A child may develop a lisp due to structural problems and other issues may be evident across the lifespan. The following images depict restriction of the frena vs. supporting function.
What are all the Acronyms?
Let’s clarify the acronyms seen in the literature and on social media. These terms also identify team members when a tethering of tissue is present or identified.
- TOTs – Tethered Oral Tissue
- IBCLC/CLC – Individual/International Board Certified Lactation Consultant; if breastfeeding is an issue, this is one professional to consult.
- SLP – Speech Language Pathologist; professionals who have training in feeding, speech, and oral sensory motor function. Can have training and/or a certification in orofacial myology.
- OT – Occupational Therapist; can be TOTs informed and can assist in posture and alignment of the body, oral motor dysfunction, and body work such as craniosacral therapy or myofascial release.
- PT – Physical Therapist; can be TOTs informed and have continuing education in craniosacral therapy, myofascial release, or more. There can be torticollis with tongue ties and PTs are essential practitioners in this area.
- RDH -Registered Dental Hygienist; can be trained in orofacial myofunctional therapy.
- OMD -Orofacial Myofunctional Disorder; one or more of the following can be an OMD: abnormal tongue resting posture, teeth grinding, lip incompetency and/or noxious oral habits, nasal breathing issues, tongue thrust swallowing, chewing difficulties, or oral placement issues related to speech.
- OMT – Orofacial Myofunctional Therapy; a treatment modality used to treat OMDs. This is not a profession.
- COM – Certified Orofacial Myologist; SLPs can become a COM, which is an extensive process involving clinical and written exams and continuing education requirements to maintain certification.
- ENT – Ear, Nose, and Throat doctor or otolaryngologist. An ENT may assess structure, complete a release, and/or to assess an airway.
- Dentist/Orthodontist – professionals on TOTs team for assessment and intervention.
What to do when Tongue Ties or TOTs are Present:
In infancy, a pediatrician can refer to IBCLC, SLP, etc. A diagnosis of TOTs does not immediately mean a release is necessary. An assessment of function will determine intervention. A speech language pathologist can conduct this assessment and be vital in pre-op care, post-op care, and functional therapy, whether oral sensory motor or orofacial myofunctional (only after the age of four). Following assessment, a release is considered with relation to age and the severity of the restriction both in classification and in function. A dentist or ENT may release a tie via laser or scissors. They will prescribe stretches to complete after the procedure, and an SLP can complete treatment in collaborative care if trained accordingly.
The Takeaway
In conclusion, when researching a proper assessment of oral structures with possible restrictions, consult professionals knowledgeable in the area, whether dentist, SLP, PCP, IBCLC, or ENT. Function is a determining factor for the indication to release or not. Navigating TOTs is a team effort in evaluation and treatment. A speech language pathologist is a professional that can be instrumental in oral motor development, feeding, and speech across the lifespan, and orofacial myology after the age of four. Choose a team wisely! Untreated oral ties can lead to a host of problems, including dental and orthodontic issues such as altered jaw and teeth development, breathing issues, reflux, head and neck pain, chronic jaw issues and/or difficulty chewing, poor dental hygiene, digestive issues, sleep apnea, and speech issues.
If you are struggling breastfeeding, it may not be related to TOTs. Check out What Exactly is a Good Latch? for breastfeeding tips.
